 A retained placental fragment is possible, but there is no evidence for this in the scenario. Disseminated intravascular coagulation is typically associated with premature separation of the placenta, a missed early miscarriage, or fetal death, none of which is evident in this scenario. Conditions that contribute to uterine atony include having received deep anesthesia or analgesia and a prior history of postpartum hemorrhage. Oxytocin is the most effective treatment for postpartum hemorrhage, even if already used for labor induction or augmentation or as part of active management of the third stage of. 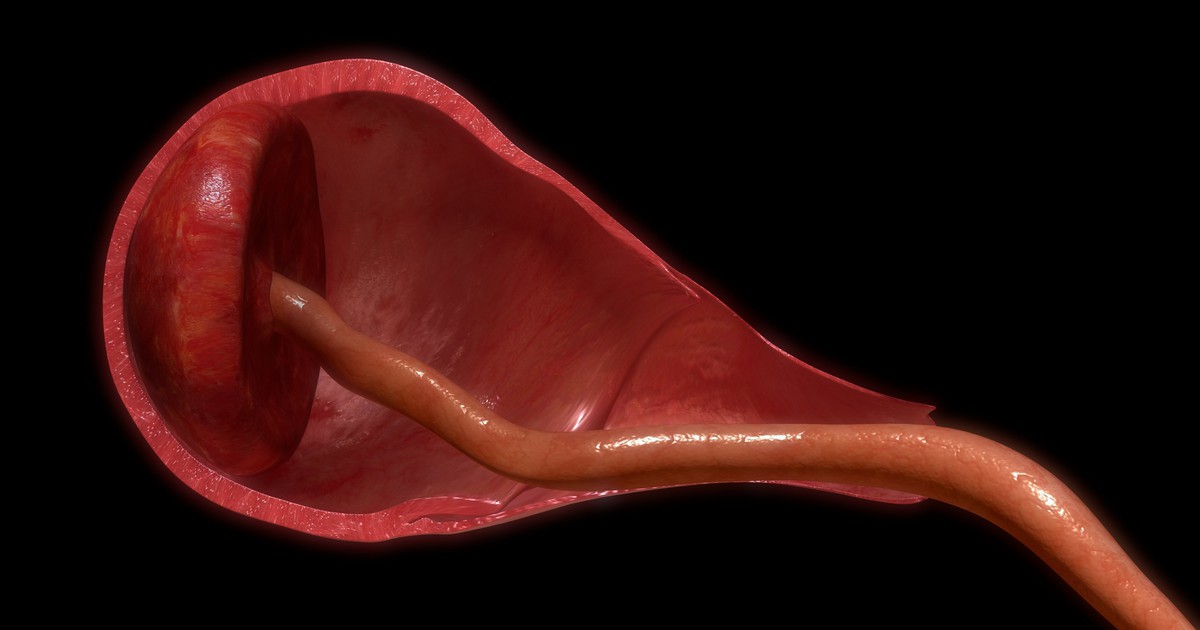
Uterine atony, or relaxation of the uterus, is the most frequent cause of postpartum hemorrhage it tends to occur most often in Asian or Hispanic woman. Blood transfusion, to replace the loss blood and fluids. Removal of placenta pieces that remain in the uterus. 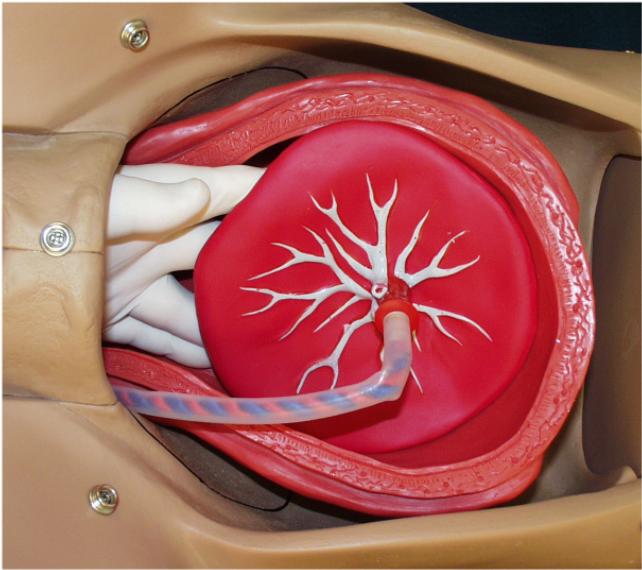
Treatment: After delivery massage the mother’s abdomen to help it contract. Numerous common and uncommon findings of the placenta. Retained parts Retained Placental fragments. Uterine atony, trauma, retained placenta fragments, coagulopathy. Fortunately, this bleeding ordinarily occurs immediately after detachment of the placenta, when the primary care provider is still in attendance. Tissue may be retained because of abnormal lobation of the placenta or because of placenta accreta, placenta increta or placenta percreta. Er of priority): Nursing Analysis/ Priority Diagnosis: Ineffective tissue perfusion. Because this is arterial bleeding, it is brighter red than the venous blood lost with uterine atony. 
If the artery is torn, the blood loss may be so great that blood gushes from the vaginal opening. Cervical laceration Explanation: Lacerations of the cervix are usually found on the sides of the cervix, near the branches of the uterine artery. 
0 Comments
Leave a Reply. |
 RSS Feed
RSS Feed
